The Joint Commission Environment of Care standard EC.02.03.03 requires hospitals to conduct regular, varied fire drills, and to routinely evaluate the effectiveness of the procedure, fire safety equipment, building features, and staff response. All drills and critiques must be documented.
Hospital Fire Drill Procedure
Hospitals don’t require full evacuation due to the size and nature of the facility, as well as the safety of the patients and staff, but there are many other protocols that determine where patients, visitors, staff, and other occupants in hospitals are supposed to go — or not go — during a fire emergency.
Practiced adherence to the fire response plan in the form of fire drills ensures staff are confident in the event of a fire and can remove patients from harm’s way and manage the situation effectively.
During a fire drill, hospital staff must enact the fire response plan as if a real fire threat is present.
What’s in a Hospital Fire Response Plan?
A hospital fire response plan will include a general plan to move patients and staff to safety as well as specific information that is directly related to the facility structure, staff roles, and more.
Every hospital should have a written fire response plan that includes when and how to sound and report fire alarms, how to contain smoke and fire, how to use a fire extinguisher, and how to evacuate areas of refuge. Staff should be trained in each of these areas, and have their knowledge tested with regular but varied fire drills.
When is the Hospital Fire Response Plan Used?
The hospital fire response plan should be enacted in situations of:
- Fire alarm activation, unless announced test
- Fire or suspected fire
- Fire drills
- Fire preparedness training
General Fire Response Plan for Hospital Fire Drills
A general fire response plan follows the RACE acronym with the additional steps of Relocation and Evacuation to protect patients in a hospital setting. Let’s go through it step-by-step.
R
Rescue persons from the room or area. Notify the nurses’ station to get assistance. Move all people away from where fire, smoke, or the strong smell of smoke exists. Assist ambulatory patients out of the room and use a wheelchair, ordinary chair, blanket drag, or lift and carry with other staff members to move non-ambulatory patients.
A
Activate the alarm. The alarm may release an audible signal, announce code red, or chime to alert staff without frightening patients and visitors. Do not shout fire, as this can cause panic. Pull the nearest alarm to mark to help the fire department to where the fire danger is present.
C
Close doors to minimize the spread of fire and smoke. All doors should be closed as quickly as possible, even if no smoke is visible. Patients not in harm’s way should be returned to their rooms with closed doors.
E
Extinguish the fire if it is safe to do so. Use a fire extinguisher and follow the PASS procedure (press, aim, squeeze, and sweep). If the situation feels unsafe, close the door and wait for the fire department to arrive.
Relocation and Evacuation
In cases where the fire spans multiple rooms, patients must be removed from those adjacent to the fire area to areas beyond fire and smoke barriers.
Elevators should not be used where the fire is located. If an elevator is required to move a patient to another floor for care, it is acceptable to use an elevator in an adjacent building that is separated from the fire.
All staff and patients should remain where they are during an alarm or drill, except for the designated response team. This limits the opening of doors to minimize smoke and fire spread. All staff will remain in their zone and only open doors to relocate patients when instructed.
Do not turn off oxygen except when instructed by the fire department, and then only after all oxygen-dependent patients have been provided with portable oxygen or relocated where they can receive care.
Priorities for relocation and evacuation:
- Ambulatory patients
- Non-ambulatory patients
- Critical patients
- Patient records to travel with the patient when possible
Who’s Involved in Hospital Fire Drills?
Hospital fire drills are meant to involve staff only, without startling patients. Since the drills are unannounced, staff have the opportunity to practice calm organization and patient reassurance in addition to their fire emergency response.
Still, there are some exceptions with conducting fire drills to minimize disruption of patient care and healing. For example, if the drill takes place between 9 pm and 6 am, the audible alarm can be kept silent. Also, in critical care areas, no audible alarms may be used to prevent risk to sensitive patients.
Individual roles during a fire or fire drill:
- Physicians, including residents and interns, if attending a patient, will remain in the room with the patient until the conclusion of the fire drill or emergency. Physicians in patient care areas that are not attending a patient should report to a nursing station to be available in case of a medical emergency. Physicians in other non-patient areas should remain in that location until the all-clear is issued.
- Hospital volunteers may assist staff with closing doors, and reassure patients of the fire response plan.
- Students will act as visitors and follow instructions to go into closed rooms during drills or emergencies unless specifically trained to act otherwise.
Hospital Fire Drill Requirements
According to the NFPA and the Joint Commission for Life Safety and Environment of Care, fire drills must be performed at least once per quarter for every shift.
To improve safety and preparedness as well as compliance with regular fire drills, the Joint Commission developed the fire drill matrix:
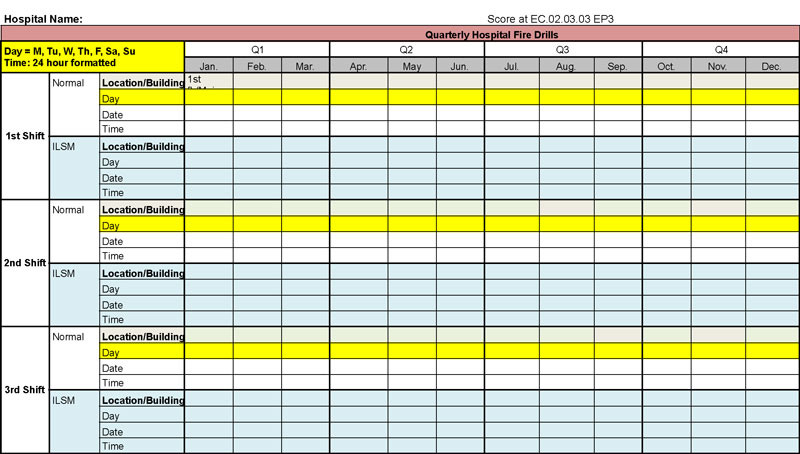
Hospital Fire Drill Matrix
The Fire Drill Matrix helps to guide the fire drill evaluation. It allows facilities to self-identify where they meet hospital fire drill requirements and where they need to improve.
This tool also makes it obvious when fire drills are scheduled or similarly grouped, such as at the same shift/time of day or same day of the week, and not conducted at varied times. Fire drills should be spontaneous and unannounced to prevent staff from anticipating them, or they risk becoming lethargic when the real thing eventually happens.
To make sure fire drills are documented and meet NFPA and Joint Commission EC standards, fire drills can be documented using this matrix, which is then given to the safety surveyor.
Hospital Fire Drill Checklist
After each fire drill, the facility should follow a clear checklist to evaluate the effectiveness of the safety protocols to find ways to improve response times, maintain a calm and efficient atmosphere, and upgrade equipment access as necessary.
An example of a hospital fire drill evaluation checklist is included below, although each facility will have different areas of preparedness to evaluate and improve.
| Hospital Fire Drill Evaluation | Yes | No |
| Did staff follow RACE to: | ||
| Rescue those in immediate danger? | ▢ | ▢ |
| Alert others of the fire and sound the alarm? | ▢ | ▢ |
| Close all doors to minimize smoke and flame transmission? | ▢ | ▢ |
| Extinguish the fire (or demonstrate proper steps of PASS)? | ▢ | ▢ |
| Were hallways and exits free of obstructions for evacuation? | ▢ | ▢ |
| Did staff maintain calm and reassure patients and visitors? | ▢ | ▢ |
| Did anyone step up to take charge of the situation? | ▢ | ▢ |
| Were patients kept in rooms when appropriate? | ▢ | ▢ |
| Do staff know where the nearest alarms are located? | ▢ | ▢ |
| Do staff know where the nearest fire extinguishers are located? | ▢ | ▢ |
| Was the fire alarm audible and visual throughout the area? | ▢ | ▢ |
| Did the fire protection system work effectively? | ▢ | ▢ |
| Do all staff understand the evacuation plan and the correct destination for patients? | ▢ | ▢ |
| Do staff know the difference between horizontal and vertical evacuation? | ▢ | ▢ |
| Is evacuation equipment accessible for the staff and patients? | ▢ | ▢ |
Make sure your facility is not only prepared for fires, but is actively doing things to prevent them as well. If you’re looking for help with your hospital or healthcare facility’s fire protection plan, give Vanguard a call. We often work with healthcare facilities and hospitals and have the experience and expertise you need.


